- Assess Your Eligibility: If your income is below 138% of the Federal Poverty Level, you likely qualify for Ohio Medicaid, which covers approximately 60% of state treatment admissions.
- Verify Network Status: Before admission, call the facility and ask specifically: “Are you in-network with my plan for residential treatment?” to avoid surprise bills.
- Document for Appeals: If denied, request a written explanation immediately. Ohio law grants you the right to an external review through the Department of Insurance.
- Know Your Parity Rights: Federal law prohibits insurers from placing stricter limits on addiction care (like session caps) than they do on medical care (like physical therapy).
Ohio’s Insurance Landscape for Rehab
Medicaid Expansion & Federal Funding
Navigating insurance for rehab in Ohio can feel complex, but understanding the funding landscape is the first step toward securing care. Medicaid expansion has played a central role in shaping access to addiction care across the state. Since the expansion, nearly 770,000 Ohioans have gained coverage, with the federal government contributing 90% of costs and the state covering the remainder4.
This influx of federal funding has had a direct impact on availability. In 2024 alone, more than $1 billion in federal dollars supported behavioral health services for Ohioans in the expansion population. This funding covers essential services including:
- Outpatient counseling and therapy.
- Psychiatric care and medication management.
- Residential drug treatment programs.
“Medicaid now serves as the main payer for substance use disorder treatment in the state, funding about 60% of admissions.”4
The Section 1115 Demonstration Waiver further expands the reach of Medicaid by allowing federal dollars to pay for residential treatment services, which historically faced funding barriers8. As of 2024, 40% of adults enrolled under Medicaid expansion had a primary mental health or substance use disorder diagnosis4, highlighting the program’s significance for individuals seeking recovery support. For Ohio families navigating insurance for rehab, Medicaid’s broad coverage and evolving federal support form the backbone of accessible, evidence-based addiction care.
ACA Plans & Employer Coverage Options
For Ohio residents, purchasing insurance through the ACA Marketplace or accessing employer-sponsored coverage offers essential pathways to evidence-based addiction treatment. In 2024, Ohio reached a record high of 477,793 individuals enrolled in Marketplace plans, reflecting growing reliance on private insurance amid ongoing behavioral health needs5.
By law, all ACA-compliant and employer health plans in Ohio must treat substance use disorder benefits as an essential health benefit. This means coverage for inpatient, outpatient, and medication-assisted treatment cannot be excluded or limited more strictly than medical care5. However, accessing care is not always straightforward. Many Ohioans face specific hurdles:
- High Deductibles: Out-of-pocket costs before coverage kicks in.
- Limited Networks: Fewer providers in rural counties compared to metro areas.
- Prior Authorization: Administrative steps that can slow treatment entry.
Employer plans, which remain prevalent in metro areas like Cincinnati, Cleveland, and Columbus, must also adhere to federal parity requirements, but actual out-of-pocket costs and access still vary by carrier and plan type. The Ohio Department of Insurance offers guidance for residents to compare plans and understand their rights, helping families make informed decisions about the best coverage for their recovery journey5.
Mental Health Parity: Your Rights Using Insurance for Rehab
The Mental Health Parity and Addiction Equity Act (MHPAEA) of 2008 established a critical protection: health insurance plans cannot impose stricter limitations on behavioral health and addiction disorder benefits than they do on medical and surgical benefits. This federal law applies to most group health plans and insurance policies, including those offered through Ohio employers and the Health Insurance Marketplace.
Under parity laws, insurance companies must provide equal coverage across several key areas. To understand if your plan is compliant, compare how it treats medical conditions versus addiction treatment:
| Feature | Medical/Surgical Example | Behavioral Health Requirement (Parity) |
|---|---|---|
| Treatment Limits | Unlimited physical therapy sessions for a knee injury. | Cannot limit substance use counseling to 10 sessions per year. |
| Prior Authorization | No pre-approval needed for 3 days of hospital recovery. | Should not require pre-approval for 3 days of residential detox. |
| Cost Sharing | $30 copay for a cardiologist visit. | Copay for a psychiatrist or addiction counselor must be comparable (e.g., $30). |
Ohio residents have additional protections under state law. Ohio Revised Code mandates that health insurance policies covering hospital and medical expenses must also cover the diagnosis and treatment of psychiatric conditions and chemical dependency disorders. Despite these protections, parity violations remain common. According to federal investigations, approximately one-third of insurance claims denials for behavioral health services violate parity requirements.
Insurance companies may disguise discriminatory practices through complex medical necessity criteria, excessive utilization reviews, or narrow provider networks. The Ohio Department of Insurance receives hundreds of behavioral health parity complaints annually from Ohio residents. If you suspect a violation, you have avenues for recourse:
- File an internal appeal with the insurance company.
- File a complaint with the Ohio Department of Insurance.
- For federal plans, submit complaints to the U.S. Department of Labor.
Coverage Across Treatment Levels in Ohio
Detox, Residential & PHP Programs
Ohio residents seeking detox, residential, or partial hospitalization (PHP) programs have several insurance options, but coverage specifics vary by insurer and plan. Medicaid remains the primary payer for addiction treatment in the state, funding about 60% of admissions, with federal Section 1115 Waiver dollars allowing for expanded access to residential programs that previously faced funding restrictions8.
For those with private insurance or ACA Marketplace plans, state and federal law require coverage for inpatient substance use disorder services as essential health benefits. However, families should be aware of the typical requirements for these intensive levels of care:
Click to view Level of Care Requirements
- Detox: Generally covered if “medically necessary” (e.g., risk of seizure). Prior authorization is frequently required.
- Residential Treatment: Provides 24-hour support. Beds may be limited in rural counties. Documentation of failed outpatient attempts is often requested by insurers.
- Partial Hospitalization (PHP): Intensive therapy (6-8 hours/day) while living at home. Covered when clinical guidelines are met.
Families in regions like the Miami Valley, Northeast Ohio, and the Appalachian counties should check with both their insurer and the treatment provider to confirm in-network status and any pre-approval steps.
IOP, Outpatient & MAT Services
Intensive outpatient programs (IOP), standard outpatient care, and medication-assisted treatment (MAT) are vital support options for Ohioans looking to rebuild their lives in the community. Insurance for rehab in Ohio, whether through Medicaid, ACA Marketplace, or employer-sponsored plans, must cover these services as essential health benefits under federal law5.
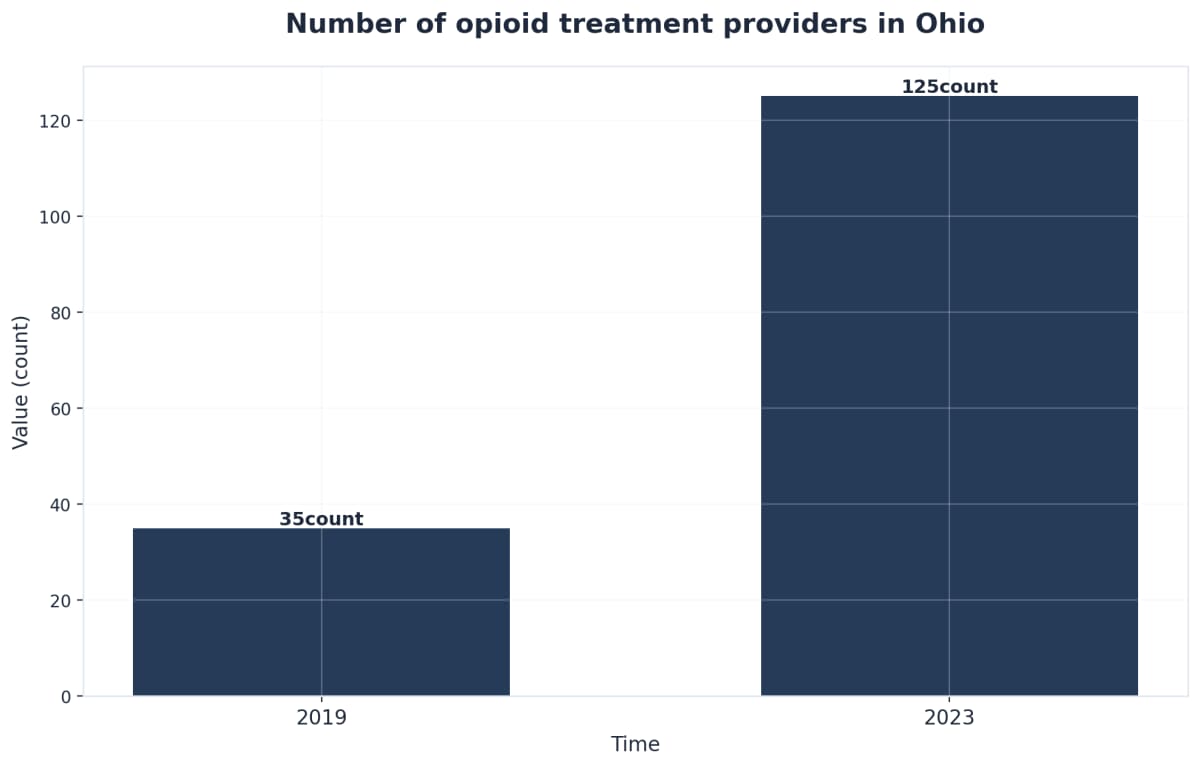
Medicaid is especially crucial, funding the majority of outpatient and MAT admissions statewide. It has also expanded peer support coverage in recent years to address both substance use and broader mental health challenges4. For MAT—such as buprenorphine, methadone, or naltrexone—Ohio has increased access by growing the number of opioid treatment providers from 35 in 2019 to 125 in 20231. Still, practical barriers remain:
- Prior Authorization: May delay access to specific medications.
- Network Limitations: Restricted access in rural counties and smaller cities like Lima or Marietta9.
Families should work closely with insurers and treatment providers to verify coverage, clarify any pre-authorization steps, and ensure the program is in-network.
Navigating Prior Authorization & Denials
One common way parity violations manifest is through excessive prior authorization requirements that create barriers to addiction treatment not applied to medical/surgical care. Insurance companies often require prior authorization before approving coverage for addiction treatment. This process involves submitting clinical documentation to demonstrate medical necessity before services begin.
While this step can feel like an obstacle when someone needs immediate help, understanding the process helps families and individuals advocate more effectively for timely care. Ohio law requires insurers to make authorization decisions within specific timeframes:
- Standard Requests: Decision within 15 days.
- Urgent Requests: Decision within 72 hours.
Denials happen for various reasons: insufficient documentation, disagreement about the appropriate level of care, or claims that treatment isn’t medically necessary. A denial doesn’t mean the end of the road. Every insurance plan must provide a clear appeals process. If you face a denial, follow this action plan:
- Request the Reason: Ask for the specific clinical reason for the denial in writing.
- First-Level Appeal: Have your provider submit additional documentation (assessments, history of overdose, failed outpatient attempts).
- Peer-to-Peer Review: Request that your doctor speak directly to the insurance company’s medical director.
- External Review: If internal appeals fail, file for an external review through the Ohio Department of Insurance.
Time matters in recovery. Families should ask treatment providers about assessment appointments that can begin while authorization is pending. Providers experienced in working with insurance companies can advocate directly with insurers, leveraging their knowledge of medical necessity criteria to strengthen authorization requests.
Regional Considerations & State Resources
When navigating insurance challenges—from prior authorization delays to claim denials—Ohio-specific resources can provide critical support. The Ohio Department of Mental Health and Addiction Services (OhioMHAS) oversees a comprehensive system of care throughout the state’s 88 counties. Each region has designated Alcohol, Drug Addiction and Mental Health Services (ADAMHS) Boards or Community Mental Health Boards.
These boards are vital for local support. They can:
- Help individuals navigate insurance coverage questions.
- Advocate during disputes with insurers over medical necessity.
- Connect residents with providers who accept specific plans.
Ohio’s Medicaid program, which covers approximately 3 million residents, includes comprehensive addiction treatment benefits protected under federal parity requirements. For those with Medicaid managed care plans through providers like Buckeye Health Plan, CareSource, Molina Healthcare, Paramount, or United Healthcare Community Plan, prior authorization requirements may vary by plan. It is essential to verify specific procedures with the managed care organization.
Geographic location within Ohio may influence treatment options and insurance network availability. A Cleveland resident may have 15 in-network providers within a reasonable distance, while someone in rural Appalachian Ohio may have only two. Urban areas like Columbus, Cleveland, and Cincinnati typically offer more in-network providers, while rural communities may have fewer options but can access telehealth services that many Ohio insurance plans now cover.
Frequently Asked Questions
What happens if Ohio’s Medicaid expansion ends?
If Ohio’s Medicaid expansion ends, nearly 770,000 Ohioans could lose insurance coverage for vital treatment, including outpatient counseling, psychiatric services, and residential care4. Medicaid currently funds about 60% of substance use disorder treatment admissions in the state, making it the primary safety net for individuals seeking recovery4. Without expansion, Ohio would either need to replace over $1 billion in annual federal funding or face significant cuts to behavioral health services. This would especially impact low-income residents and those in rural areas, who rely on Medicaid as their main insurance for rehab. Loss of expansion would likely mean fewer treatment options and higher barriers to care.
Does Tricare cover addiction treatment at Ohio facilities?
Tricare, the health insurance program for military members and their families, does cover addiction treatment at many Ohio facilities. Tricare plans generally include coverage for inpatient, outpatient, and medication-assisted treatment when medically necessary and provided by an approved or certified provider. Most major Ohio cities, including Columbus, Dayton, and Cleveland, have Tricare-authorized treatment centers. Individuals should confirm with both Tricare and the Ohio facility that the provider is in-network and accepts Tricare for insurance for rehab. Coverage details, such as copays and prior authorization requirements, may vary by plan. Always verify benefits in advance to ensure a smooth admission process.
Can my insurance company require step therapy before covering medications for opioid use disorder in Ohio?
Yes, insurance companies in Ohio can require step therapy before covering certain medications for opioid use disorder, even though federal mental health parity laws are designed to ensure equal treatment for behavioral health and medical conditions. Step therapy means your insurer may ask you to try one or more alternative medications first before approving the medication your provider recommends9. This practice is considered a non-quantitative treatment limitation (NQTL) and, while legal, may cause delays or barriers to starting evidence-based care. If you feel step therapy is being used unfairly with your insurance for rehab, you can appeal the decision or seek help from the Ohio Department of Insurance.
How do I verify if a treatment facility in Cleveland or Columbus is in-network with my insurance?
To confirm if a treatment facility in Cleveland or Columbus is in-network with your insurance, start by contacting your insurance company directly for a list of approved providers in your area. You can also use your insurer’s online portal, which typically allows you to search by city or ZIP code. Many Ohio health plans have provider directories that are updated regularly. It’s wise to call the treatment facility as well to verify they accept your specific insurance for rehab, as network status can change. The Ohio Department of Insurance offers guidance and tools to help residents compare network participation and coverage options5.
What can I do if my insurance denies coverage for residential treatment in Ohio?
If your insurance denies coverage for residential treatment in Ohio, you have the right to request a written explanation of the denial. Start by asking your provider for additional clinical documentation that may strengthen your case. You can appeal directly to your insurance company, and request a peer-to-peer review with their medical director if needed. If the appeal is unsuccessful, Ohio law allows you to seek an external review through the Ohio Department of Insurance or file a formal complaint5. These steps help many Ohio families secure access to residential care under their insurance for rehab.
Are peer support services covered by insurance in Ohio?
Yes, most insurance plans in Ohio—including Medicaid, ACA Marketplace, and many employer-sponsored policies—cover certified peer support services for substance use and mental health recovery. As of 2025, Ohio Medicaid expanded coverage to include Adult, Family, and Youth/Young Adult peer supporters, connecting individuals with trained peers who share lived experience and provide local insight4. Private insurance coverage for peer support may vary, so it’s important to confirm benefits with your plan. Using insurance for rehab in Ohio, peer support is increasingly recognized as an essential part of recovery, especially in regions facing provider shortages and workforce gaps.
Will my employer know if I use my insurance for substance use treatment?
In Ohio, your employer typically does not receive details about your specific health care claims, including substance use treatment, when you use insurance for rehab. Health privacy laws like HIPAA require insurers to keep your medical information confidential. If you use employer-sponsored insurance, your employer might see overall plan usage or costs, but not the nature of your treatment. Only in rare cases—such as leave requests under FMLA or disability benefits—would you need to disclose treatment details, and even then, information is limited. Ohioans can feel confident that seeking help through insurance for rehab remains a private matter protected by both state and federal law5.
Choosing the Right Path Forward in Ohio
Armed with knowledge of parity rights and available resources, Ohio residents can make informed treatment decisions that maximize their insurance benefits. Selecting an appropriate treatment facility represents a deeply personal decision that depends on individual circumstances, health needs, and recovery goals. Ohio residents have access to a diverse range of options, from residential programs offering intensive support to outpatient services that allow individuals to maintain work and family commitments while receiving care.
When evaluating facilities, insurance-specific considerations should guide the selection process. Before committing to a program:
Verify the facility’s in-network status with your insurance carrier.
Obtain written confirmation of coverage details, including deductibles and copayments.
Ask prospective facilities about their experience navigating insurance appeals.
Recovery is rarely a linear process, and the most effective path forward often involves ongoing support beyond initial treatment. Ohio’s network of recovery support services, peer mentorship programs, and community resources can provide crucial assistance during the transition back to daily life. Ohio residents facing insurance barriers should remember that federal and state parity laws exist specifically to protect access to necessary mental health and addiction treatment. By understanding these legal protections, documenting coverage denials, and advocating persistently through available channels, you can assert your rights to equitable care.
Connect with Arrow Passage Recovery today for more information and support on your path to a happier, healthier, substance-free life.
References
- Medications for Substance Use Disorders – SAMHSA. https://www.samhsa.gov/substance-use/treatment/options
- Vital Statistics Rapid Release – Provisional Drug Overdose Data – CDC. https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm
- Drug Overdose – Ohio Department of Health. https://odh.ohio.gov/know-our-programs/violence-injury-prevention-program/drug-overdose/
- Access to mental health and substance use disorder treatment – Health Policy Institute of Ohio (HPIO). https://www.healthpolicyohio.org/our-work/publications/access-to-mental-health-and-substance-use-disorder-treatment
- Health Insurance Guide – Ohio Department of Insurance. https://insurance.ohio.gov/consumers/health/health-insurance-guide
- Mental Health Parity – Ohio Department of Behavioral Health. https://dbh.ohio.gov/wps/portal/gov/mha/about-us/priorities/mental-health-parity
- Prior Authorization Requirements – Ohio Department of Medicaid. https://medicaid.ohio.gov/PROVIDERS/PriorAuthorizationRequirements.aspx
- Substance Use Disorder 1115 Demonstration Waiver – Ohio Department of Medicaid. https://medicaid.ohio.gov/wps/portal/gov/medicaid/families-and-individuals/substance-use-disorder-1115-waiver
- 2025 Ohio Mental Health Parity Annual Report – Ohio Legislative Service Commission. https://www.lsc.ohio.gov/assets/organizations/legislative-service-commission/monthly-agency-reports/agency-reports/files/mentalhealthparityannual2025.pdf
- Where Ohio Stands on Insurance Coverage of Mental Illness and Substance Use Disorders – Community Solutions. https://www.communitysolutions.com/resources/pursuit-parity-ohio-stands-insurance-coverage-mental-illness-substance-use-disorders

