What is Fentanyl?
Overdose, Side Effects, and Half-Life

What is Fentanyl?
Overdose, Side Effects, and Half-Life
Introduction
Fentanyl-involved overdose deaths continue to rise in the US. In 2016, 29% of all drug overdose deaths mentioned the involvement of fentanyl.1
Likewise, of 70,237 drug overdose deaths in 2017, more than two-thirds involved opioids. Synthetic opioids, including fentanyl, accounted for nearly 60% of all opioid overdose deaths.2
The death rate involving fentanyl and similar drugs increased by a whopping 45% from 2016 to 2017.2 With this, fentanyl has overtaken heroin as the leading cause of drug overdose deaths in the US.
Illicitly manufactured fentanyl is the major driver of overdose fatalities in recent years.
What is Fentanyl?
Fentanyl is a potent synthetic opioid available only on a prescription. It is a member of a group of pain medications known as narcotic analgesics.
Different forms of the drug are currently available. These include oral tablets, lozenges, and lollipops. Nasal sprays, transdermal patches, and solution for injection are also available.
Narcotic analgesics work by increasing the levels of a brain chemical – dopamine. Increased dopamine levels help relieve pain, promote euphoria, and decrease pain perceptions.
Fentanyl is 50 to 100 times more potent than morphine.3
Its therapeutic index (TI) is nearly four times that of morphine and over 50 times that of meperidine. TI measures the relative safety of a drug.4 The greater the value of TI, the safer is a drug.
Fentanyl History: Revisiting the Birth of America’s Top Killer Drug
Both morphine and meperidine were well-known opioid analgesics during the early 1950s. However, both the drugs were poorly absorbed into the brain. Thus, they took longer to show the pain-relieving effects.
Early Development
Paul Janssen and his team synthesized fentanyl in 1960. They were looking for an alternative to morphine and meperidine.5 Paul was a Belgian doctor and founder of Janssen Pharmaceutica. Paul and his team were looking for more powerful and rapidly acting pain medication. Between 1953 and 1957, they developed several new molecules. The most notable of these molecules was phenoperidine.
Animal studies revealed that phenoperidine was 25 times more powerful than morphine. Likewise, it was more than 50 times more powerful than meperidine.
The Janssen Company marketed phenoperidine in many European countries but not the US since they did not have permission to market there.
In the late 1950s, the team developed several phenoperidine-like molecules.
Eventually, they developed fentanyl in 1960. Animal studies showed it was ten times more powerful than phenoperidine. Initially, only the injectable form was considered effective for pain relief.
FDA Approval
The US FDA approved fentanyl in 1968 if it was combined droperidol. In 1972, the US FDA approved a vial containing only fentanyl.
Since the 1990s, the fentanyl patch has been widely used to manage both chronic cancer and noncancer pain.
In the last two decades, over twelve fast-acting preparations have become available.
Uses of Fentanyl
Fentanyl has several uses. Doctors prescribe it for treating severe pain in cancer patients. Likewise, they also prescribe it for patients who have undergone major surgery.
It may also be used to treat chronic pain in patients who do not respond to other opioid pain medications.
As a sedative, it is used as a drip in intubated patients to assist ventilation. Sometimes, it may be used before or during surgery to calm a patient down.
Sometimes, doctors may use it in combination with antipsychotic medications to treat epilepsy.
Fentanyl Side Effects: Things to Know
Side effects may be experienced while taking prescribed doses. The side effects can be worse when someone abuses or misuses the drug.
Anyone who is taking fentanyl in the prescribed doses may experience:
- Chest pain
- Breathing difficulties such as irregular or shallow breathing
- Drowsiness
- Sudden loss of consciousness
- Mental confusion
- Severe weakness
- Yellowish or bluish discoloration of lips, fingernails, or skin
- Slow heart rate
- Dry mouth
- Nausea
- Constipation
- Reduced pupil size
- Sweating
- Unusually stiff muscles
- Problems with focus
Some people may also complain of:
- Blurry vision
- Cough
- Problems with swallowing
- Headache
- Chills
- Rapid heartbeat
- Extreme restlessness
- Hallucinations
- Changes in facial expressions
- Skin rashes
Most of these side effects usually go away on their own. However, some effects may persist and can lead to complications. If any side effects persist or become worse, talk to your doctor immediately.
The patches may cause skin rashes, itching, and swelling at the site of application.
Fentanyl Abuse and Addiction
The National Institute on Drug Abuse (NIDA) defines fentanyl abuse as “the use of fentanyl without a prescription, in a way other than as prescribed, or for the experience or feelings elicited.”6
The American Academy of Pain Medicine (AAPM) defines addiction as “a primary, chronic, neurobiological disease, with genetic, psychosocial, and environmental factors influencing its development and manifestations. It is characterized by behaviors that include one or more of the following: impaired control over drug use, compulsive use, continued use despite harm, and craving.”6
In simple terms, addiction is a long-term brain disease in which an individual compulsively uses a drug despite its harm. The pattern of drug use is continuous. Moreover, the individual has little control over its use.
Long-term fentanyl abuse can lead to its addiction. This is because it is one of the most addictive prescription drugs. However, one should keep in mind that addiction from prescription fentanyl is rare.
In most cases, addiction develops from its recreational use. The US market has been flooded with illegally manufactured fentanyl, worsening the opioid epidemic.
Fentanyl Overdose: A Quick Look at the Stats
A drug overdose occurs when an individual accidentally or deliberately consumes a large amount of the drug within a short period.
Fentanyl is a relatively safe drug. Nonetheless, overdose deaths are increasing at an alarming rate.
The rate of drug overdose deaths involving fentanyl and related substances increased by 100% each year from 2013 through 2016. In 2013, the rate was 0.6 per 100,000, whereas, in 2014, it was 1.3. Likewise, it more than doubled to 5.9 in 2016 from 2.6 in 2015. This is according to the National Vital Statistics Report. The report was published on December 12, 2018.1
The same report also noted that fentanyl overdose deaths were mentioned in:
Fentanyl Overdose Deaths 2011-2016
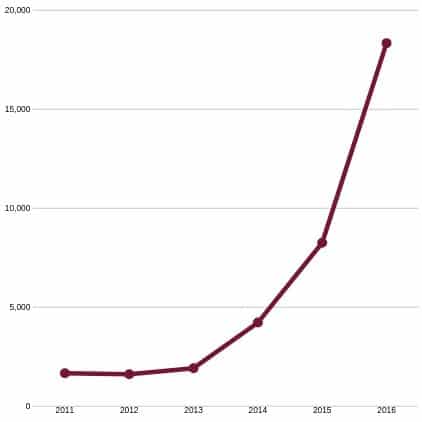
1,662 in 2011
1,615 in 2012
1,919 in 2013
4,223 in 2014
8,251 in 2015
18,335 in 2016
By the end of 2017, nine out of every ten overdose deaths in Massachusetts involved fentanyl.7
Signs
Below are the signs of an overdose8:
Sudden breathing difficulties
Confusion
Loss of consciousness
Excessive sweating and reduced body temperature
Bluish discoloration of the skin and nails
Coma and death due to impaired blood supply to the brain
Overdose Treatment and Prevention
Treatment
Naloxone is an antidote for fentanyl overdose. For better outcomes, treatment with naloxone should begin as early as possible.
Naloxone is known as an opioid antagonist. It prevents the drug from binding to opioid receptors in the body. That way, it blocks the effects of fentanyl and other opioids.
Naloxone is available without a prescription in most states in the US. Some authorities also urge people who use fentanyl or other opiates to carry naloxone with them. 9
Prevention
Strictly follow the directions for use
Do not mix fentanyl with alcohol, sleeping pills, or other medications
If you are using it for the first time, or are returning to use after detox, remember that the risk of overdose may be higher
Sources of Illegal Fentanyl
A major portion of the illegal drug comes from China.10
A thousand grams of fentanyl is available in China for about $4000. The same amount can be potentially lethal for 500,000 people.11
A 2018 study suggests the “recreational” drug market gets most of its fentanyl from two major sources.12
First, from illegal manufacturing facilities, both inside and outside the country. The manufacturers may also mix it with heroin or cocaine to increase potency.
Second, from fentanyl-containing medicines such as the patches. Drug abusers may inject or inhale fentanyl obtained from the patches. Interestingly, some may eat the whole patch or insert it into the rectum.
Keeping a patch in the mouth dramatically increases absorption into the bloodstream. That way, the contents of a 50 mg patch can produce blood levels equivalent to those produced by 5000 mg of oral fentanyl.13
Fentanyl Withdrawal Symptoms
If you have been using fentanyl for some time, stopping it abruptly can cause a set of unpleasant effects. These effects are known as withdrawal symptoms. Withdrawal symptoms indicate the dependence of an individual on a drug.
These symptoms can begin within a few hours of stopping the drug
Excessive sweating and chills
Restlessness
Nausea and vomiting
Cravings
Loss of sleep or inability to maintain sleep
Stomach or leg cramps
Runny nose
Pain in muscle and bone
Diarrhea
Unusual leg movements
Watery eyes
If you experience any of the symptoms mentioned above, talk to your doctor immediately.
Top 3 Misconceptions About Fentanyl
Myth 1 | Touching Fentanyl Can Kill You
Truth: For fentanyl to kill an individual, a sufficient amount of the drug must reach the bloodstream and brain. This is possible only after it crosses the barriers such as the skin.
However, simply touching does not allow sufficient drug to reach the bloodstream or brain. Thus, brief, accidental skin exposure is unlikely to cause toxicity.
Even if it does, toxicity develops rather slowly. This allows for post-exposure medical care if necessary.
Myth 2 | Inhaling Fentanyl Can Kill You
Truth: Inhaling fentanyl may be more dangerous than touching it. However, a brief inhalation is unlikely to cause fatal complications.
According to the American College of Medical Toxicology (ACMT) and American Academy of Clinical Toxicology (AACT),
“At the highest airborne concentration encountered by workers, an unprotected individual would require nearly 200 min of exposure to reach the medical dose of fentanyl.”14
Myth 3 | Fentanyl is Lethal Even at Low Doses
Truth: It is a relatively safe drug when used as prescribed.
When used as recommended, it is not lethal. After all, the US FDA approved it decades ago for the management of severe pain.
A drug without information is poison. However, fentanyl is a drug with dosage information. That said, illicitly manufactured fentanyl can cause death even with a low dose. No one knows the exact amount of the drug in such preparations. Thus, in such cases, accidental exposure may be fatal.
The LD50 of fentanyl is 3.1 milligrams per kilogram of body weight in rats. For monkeys, it is 0.03 milligrams per kilogram of body weight. However, researchers have not yet determined the LD50 in humans.15 LD50 is an acronym for Median Lethal Dose. It is the amount of a substance that can cause fatalities in 50% of lab animals within a certain period.
Treating an Addiction to Fentanyl
A combination of medication and behavioral therapies is usually the most effective treatment for fentanyl addiction.
Medications
Commonly used medications to treat withdrawal symptoms for fentanyl are methadone, buprenorphine, and naltrexone. Methadone and buprenorphine help reduce the severity of withdrawal symptoms and cravings. These medications work on the same brain areas as fentanyl. However, they do not produce a “high”.
A combination of buprenorphine and naloxone may also be used in some cases. Naloxone is an antidote for opioid overdose. It counteracts the effects of opioids. Using the combination reduces the risk of buprenorphine misuse.
Naltrexone is a bit different when it comes to helping with opioid addiction. It does not curb cravings or reduce withdrawal symptoms. Instead, it helps prevent relapse.
These medications are typically safe and may be used for months or years. One should not stop taking these drugs without first consulting a doctor.
Counseling and Behavioral Therapies
Counseling and behavioral therapies are non-drug approaches for addiction treatment.
They help people with substance use disorders change attitudes toward addictive behaviors. Therapy also assists in re-entering a drug-free life and sticking to a treatment plan.
Different forms of counseling are used, such as:
Individual counseling
It involves one-on-one interaction between an individual and a counselor. The counselor teaches ways to set goals, cope with cravings, and monitor progress. Besides, the individual can also discuss legal matters related to drug use.
Specific behavioral therapies used in counseling include:
Cognitive-behavioral therapy (CBT)
CBT assists in recognizing problematic thought patterns and subsequent behaviors. Once an individual recognizes behaviors they don’t like within themselves, they can learn skills to stop.
Motivational enhancement therapy (MET)
MET keeps an individual motivated throughout the treatment period. A motivated individual is more likely to stick with the treatment plan. Eventually, this leads to greater chances of recovery.
Contingency management (CM)
This approach rewards individuals for positive changes in their behavior. Rewards are crucial for strengthening the positive changes.
Group counseling
Group counseling involves a group of people who share their problems. It is a great approach for sharing problems, celebrating progress, and learning from peers.
Family counseling
Family counseling involves an individual’s partner, spouse, and any close family members. Sharing problems and discussing possible solutions with closed ones can help rebuild or strengthen relationships.
In addition to counseling, counselors can also help an individual connect to other resources. For example:
- Peer support groups, such as Narcotics Anonymous (NA)
- Spiritual and faith-based groups
- HIV testing and hepatitis screening programs
- Employment or educational supports
Inpatient and Outpatient Treatments for Fentanyl Addiction
Residential programs provide both housing and therapy. There are two main types of treatments. They are:
Inpatient programs. They provide specialized health care and treatment facilities to individuals. The individuals live in the hospital or other treatment facility during recovery and detox.
Intensive outpatient treatment. The individuals do not need to stay in the hospital. Rather, they can schedule regular visits for treatment and live at home or other sober living facility.
Key Takeaways
Deaths from fentanyl overdose are on the rise. In 2016, Fentanyl was the number one killer among drugs involved in overdose deaths.1
Majority of deaths have been linked to illicitly manufactured drug.
Fentanyl is a synthetic narcotic pain medication. It is used to treat severe pain associated with cancer and surgery.
Paul Janssen and his team first synthesized fentanyl in 1960 in Belgium.
The US FDA approved its combination with droperidol for use in America in 1968. After four years, the FDA approved fentanyl-only preparation. Currently, different forms of the drug are available.
Fentanyl is 50 to 100 times more potent than morphine.
It is very addictive and has been the major cause of overdose deaths in recent years.
Naloxone is an antidote for opioid overdose. In most states, one can get naloxone without a prescription.
Accidental, unintentional, and brief exposures are unlikely to cause toxicities.
Treatment for fentanyl addiction involves medications, counseling, or both.
The single best way to prevent an overdose is to strictly follow the doctor’s instructions.
Resources
- National Vital Statistics Reports. Drugs Most Frequently Involved in Drug Overdose Deaths: United States, 2011–2016.
- Centers for Disease Control and Prevention. Drug and Opioid-Involved Overdose Deaths — United States, 2013–2017.
- National Institute on Drug Abuse. Drug Facts. Fentanyl.
- ToxTutor. Determining the Safety of a Drug.
- The Journal of Pain. The Fentanyl Story.
- Pain. Classification and definition of misuse, abuse, and related events in clinical trials: ACTTION systematic review and recommendations.
- EuropePMC. Fentanyl shock: The changing geography of overdose in the United States.
- Your Room. Fentanyl.
- American Journal of Health-System Pharmacy. Nonprescription availability of the opioid antagonist naloxone.
- Population and Development Review. The Contemporary American Drug Overdose Epidemic in International Perspective.
- Department of Justice.
- Forensic Science International. Abuse of fentanyl: An emerging problem to face.
- Case Reports in Medicine. Management of an Oral Ingestion of Transdermal Fentanyl Patches: A Case Report and Literature Review.
- Journal of Medical Toxicology. ACMT and AACT Position Statement: Preventing Occupational Fentanyl and Fentanyl Analog Exposure to Emergency Responders.
- PubChem. Fentanyl.

