Adderall Use and Abuse

Adderall Use and Abuse
Introduction
What is Adderall?
Adderall is the brand name for a combination drug containing both amphetamine and dextroamphetamine. Both medications are synthetic stimulant drugs that act on the central nervous system. The drug works by enhancing the chemicals that act on receptors in the brain, especially dopamine and norepinephrine.1
The drugs generic name is amphetamine and dextroamphetamine mixed salts, often shortened to amphetamine salts. Other brand names that include the same mix of medications are Adderall XR (extended-release), and Mydayis.
How is Adderall Used?
For people with attention deficit hyperactivity disorder (ADHD), Adderall can help improve attention, focus, and concentration while decreasing impulsive behaviors and hyperactivity. A 2013 study found that stimulant medications help to improve episodic memory, decrease extreme emotional reactions to frustration, increase effort, and improve the ability to detect errors in work.2 This study also found that while stimulant medications improve attention and focus, they do not improve cognitive performance.
Besides ADHD, the medication is used to treat cognitive symptoms in people with neurological disorders, such as multiple sclerosis or Parkinson’s Disease. Adderall is also used to treat narcolepsy, a sleep disorder. Taking the drug during the day helps to improve levels of alertness, therefore improving the symptoms of narcolepsy.
More About Stimulants
Is Adderall an Opioid?
Considering the current focus on reducing opioid use in the United States, many people wonder if Adderall is an opioid. The answer is no. Opioids are medications that are made from opium, hence the term opioid. These medications typically have a depressant effect on the central nervous system. On the other hand, Adderall is a stimulant medication, so it has the opposite effect of opioids. Both drugs, however, can produce a euphoric “high” when taken in large doses and lead to addiction. A 2011 study found that the differences in how both drugs affect the dopamine receptors in the brain lead to different mechanisms of addiction and different addictive behaviors. 3
The Stimulant Epidemic
According to experts, the United States is currently experiencing a stimulant epidemic that is just as dangerous as the opioid epidemic. The National Emerging Threat Initiative reports that between 2014 and 2018, for every kilogram of heroin seized by drug enforcement officials, 15 kilograms of stimulants were seized.
Additionally, the Centers for Disease Control (CDC) reported that deaths from both illegal and prescription stimulants increased by almost 30% between 2016 and 2017. 4 While opioid overdoses can be reversed when treated quickly with the medication Narcan, there are no reversal drugs for stimulant overdoses. While stimulants like Adderall are not the same as opioids, their abuse is just as concerning as the misuse of opioids.
Side Effects of Adderall
The positive side effects of Adderall include an increased level of alertness and wakefulness, increased focus, and a calm demeanor. Other side effects include:
Nervousness
Restlessness
Headaches
Dizziness
Insomnia
Dry mouth
Hoarseness
Changes in vision
Slowed speech
Serious Side Effects Include:
Fever
Weakness
Numbness of the limbs
Shaking or ticks
Seizures
Increased depression or anxiety
Increased heart rate
Increased blood pressure
Blurred vision
Chest pain
Fainting
Shortness of breath
Confusion
Hallucinations
Increased aggression
Delusions
Individuals who experience these serious side effects should seek medical attention immediately.
Medical Conditions That Increase the Risk of Side Effects
Some pre-existing medical conditions increase the risk of developing side effects. These medical conditions include:
A history of cardiac conditions including heart attack or heat defects
Circulatory problems
Glaucoma
Depression/anxiety
Drug addiction
Allergy to stimulant medications 5
High blood pressure
History of stroke
Hyperthyroidism
Seizures
Recent use of monoamine oxidase inhibitors
These serious side effects can also be present during an overdose.
How Long Does Adderall Last?
In general, the effects last 4 to 6 hours. The actual length of effect is dependent on factors including weight, metabolism, and the dosage of medication. Adderall XR is formulated to release more slowly in the body, so it can last up to 12 hours.
Testing for Adderall Use
Though the drug is thought to leave the body quickly, it can be detected through metabolic tests for some time after the effects have worn off. The body absorbs Adderall through the gastrointestinal tract, it’s broken down by the liver, and then flushed out of the body by the kidneys. Adderall can show up in blood tests up to 46 hours after the last use and can be identified in the urine up to 72 hours after the last use. It can also be detected by testing hair up to 3 months after the last use, although this is not a common method of testing.6
Is Adderall Bad for You?
When taken in prescribed doses for medical conditions like ADHD, Adderall is a safe medication. However, when it is taken without a prescription for reasons other than a medical condition, it is not safe. Many people buy it off the street and self-medicate under the false belief they can “get more done” or “stay awake to study.” While it might help people stay awake, it will not improve the cognitive functions to get more work done.
People who regularly take Adderall for recreational purposes find that they need more and more of the drug to achieve the same effects. This is called tolerance. At higher doses, Adderall’s effect on the cardiovascular system could cause racing heartbeat, headaches, high blood pressure, or even a heart attack.7 These and other side effects from Adderall are dangerous and not worth the risk.
Long-Term Effects of Adderall Use
Like other stimulant medications, Adderall suppresses the appetite. In children with a long-term prescription, this can lead to decreased nutritional intake and slowed growth. Long-term use can also lead to tolerance of the medication. Tolerance can lead to dependence on the drug and withdrawal if Adderall is stopped suddenly.
Addiction to Adderall
At low, medically-safe prescription doses, Adderall is typically not addictive. However, high doses of it can lead to addiction. It is classified as a Schedule II controlled substance by the U.S. Controlled Substances Act because of its addictive properties.
People with an Adderall use disorder typically take higher doses to achieve a stronger effect from the drug. This is followed by a “crash” after the drug wears off, prompting more use, more often. The cycle leads to tolerance and a higher risk of overdose. People who take prescription doses of the drug for long periods are also at a higher risk of developing an addiction. This includes children and adolescents who have been prescribed the drug by their pediatricians to help address ADHD.
Rates of Misuse and Abuse
2006-2011
Adderall misuse has significantly increased over the past 15 to 20 years. A study published in The Journal of Clinical Psychiatry in 2016, found that Adderall abuse occurred primarily in young adults. The study showed that between 2006 and 2011, non-medical use of the drug increased in adults age 18 to 25 by 67 percent. During the same period, emergency room visits associated with misuse of the drug increased 156 percent.
Researchers found that young adults misusing the drug primarily got it from family and friends, many of whom possessed prescriptions for it. Young adults who misuse the drug are often college students who view it as a study aid.8
2015-2018
More recent statistics on Adderall misuse support the findings of this study. Statistics from the National Survey on Drug Use and Health (NSDUH) highlight the misuse of prescription stimulant medication, from 2015 to 2018. The following graph shows the percentage of adults who misused prescription stimulant medications in this time, broken down by age group.9
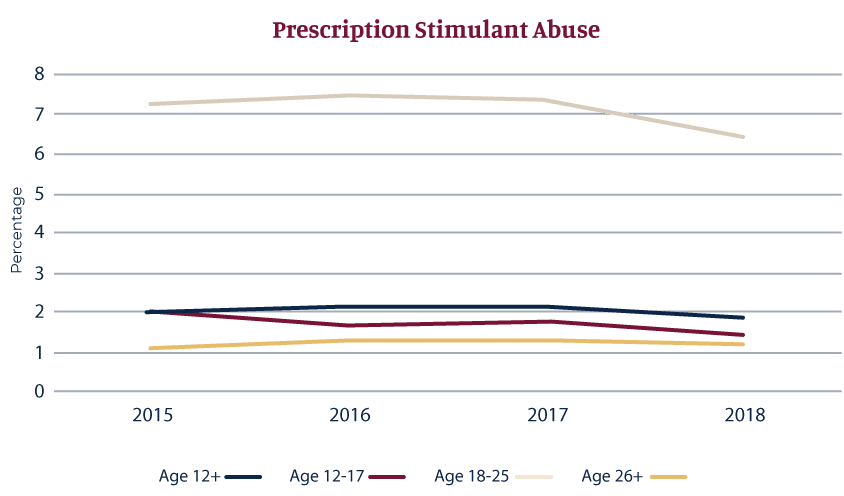
As the graph shows, adults age 18 to 25 misused prescription stimulant medications at a rate of 5 to 6 percent higher than other adult age groups. The Substance Abuse and Mental Health Service Administration (SAMHSA) has also found that full-time college students are twice as likely as non-students to have misused Adderall. Since the drug is cheap and easily accessible, it is used at parties to offset the effects of alcohol. Those who mix the drug with alcohol may end up drinking more alcohol, which can result in alcohol poisoning.
Treatment for Adderall Addiction
Step One: Detox
Similar to other addictive substances, treatment for Adderall addiction requires a period of detoxification, or “detox,” where the drug is removed from the body. Detox from the drug should be medically managed by a physician, as withdrawal symptoms can be uncomfortable and severe symptoms can be dangerous. If withdrawal symptoms are mild, a person can complete detox at home with physician supervision. If symptoms are severe or life-threatening, detox may need to be completed in an inpatient medical setting.
Step Two: Ongoing Recovery
Once detox is completed, rehabilitation for Adderall addiction may begin. This can take place in either an inpatient or outpatient setting, depending on the length and severity of the addiction. There are not currently any medications approved for the treatment of Adderall addiction.
People who are recovering from Adderall addiction may benefit from a treatment model called The Matrix Model.10 This model involves intensive outpatient treatment that utilizes a variety of therapeutic methods including:
- Individual counseling
- Relapse prevention groups
- Educational groups
- Social support groups
- Urine and breath testing
The Matrix Model program typically lasts 16 weeks. Treatment is non-confrontational and instead focuses on recognizing and changing addictive behaviors. This style of treatment is very effective for people recovering from addiction to stimulant medications.
Get Help for Long-Term Misuse of Adderall
Adderall, though commonly used to treat ADHD, is a drug that should not be misused or abused. Long-term misuse can cause life-threatening symptoms and lead to addiction. If you or someone you know is struggling with Adderall misuse or addiction, help is available and recovery is possible.
Resources
- Legg, Timothy J. “Effects of Adderall on the Body.” Healthline, Healthline Media, 25 Sept. 2017.
- Advokat, Claire, and Mindy Scheithauer. “Attention-Deficit Hyperactivity Disorder (ADHD) Stimulant Medications as Cognitive Enhancers.” Frontiers in Neuroscience, Frontiers Media S.A., 29 May 2013.
- Badiani, Aldo, et al. “Opiate versus Psychostimulant Addiction: The Differences Do Matter.” Nature Reviews. Neuroscience, U.S. National Library of Medicine, 5 Oct. 2011.
- Goodman, Brenda. “Experts Warn of Emerging ‘Stimulant Epidemic.‘” WebMD, WebMD, 3 Apr. 2018.
- Lillis, Charlotte. “Adderall: Uses, Side Effects, and Dosage.” Medical News Today, MediLexicon International, 3 July 2019.
- Hersh, Erica. “How Long Does Adderall Stay in Your System?” Healthline, Healthline Media, 3 Oct. 2019.
- Puniewska, Maggie. “What Are the Effects of Adderall If You Don’t Have ADHD?” Vice, Vice Media LLC, 18 Nov. 2016.
- Hub Staff Report. “Adderall Abuse on the Rise among Young Adults, Johns Hopkins Study Suggests.” The Hub, Johns Hopkins University, 16 Feb. 2016.
- Lipari, Rachel N., and Eunice Park-Lee. “Key Substance Use and Mental Health Indicators in the United States: Results from the 2018 National Survey on Drug Use and Health.” Substance Abuse and Mental Health Service Administration, U.S. Department of Health & Human Services, 20 Aug. 2019.
- Jeanne L. Obert, Michael J. McCann, Patricia Marinelli-Casey, Ahndrea Weiner, Sam Minsky, Paul Brethen & Richard Rawson (2000) The Matrix Model of Outpatient Stimulant Abuse Treatment: History and Description, Journal of Psychoactive Drugs, 32:2, 157-164.

